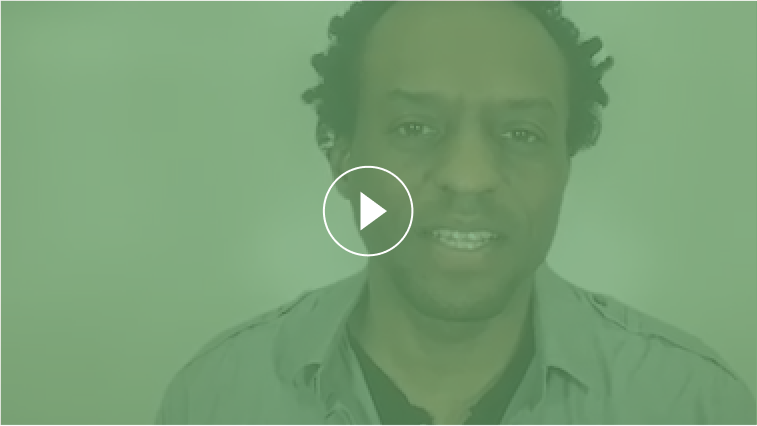
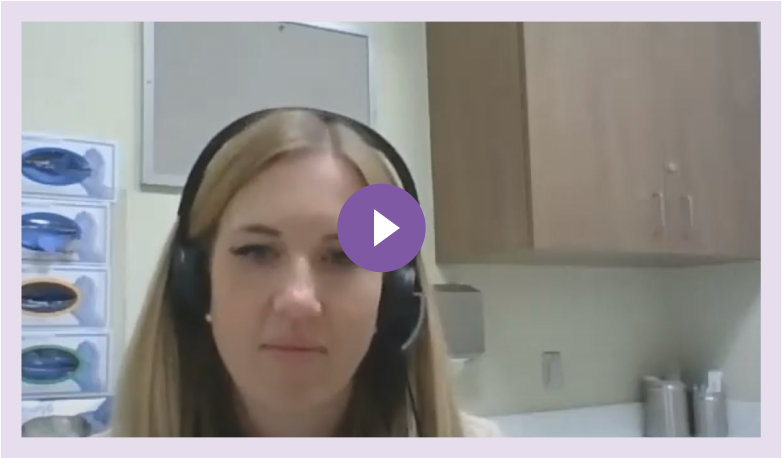
Adam, 40, who is the father to 4-year-old Daniel, sees a pediatrician due to Daniel’s persistent nighttime cough. Adam has never had to answer an ACE questionnaire before for Daniel. He is wondering what these questions have to do with his son’s asthma. What can a parent do to support their children if they have experienced ACEs?
What Adam Is Thinking as the ACEs Screening Is Introduced
- What do these questions have to do with Daniel’s cough?
- I want Daniel to lead a happy, healthy and stable life.
- Why does the health care team think there is stress in the home and want to do a home visit? Do they think I’m doing something wrong?
Learning Objectives:
- Recognize approaches to inquiring about and validating adversity, distress and strengths in ways that support healing
- Identify words and practices within the TRIADS framework that resonate with your own approach to health care
- Practice applying the TRIADS framework
Watch & Learn
5 min
What Happens Next
Adam tells Dr. Gantz that talking with his son about family stressors improved his son’s symptoms.
Finding Your Own Words
Below are some commonly asked questions and an example response. The aim is to help you find your own words when communicating with your patients about the ACEs screening.
My child is so young. How could these traumatic experiences affect my child’s asthma?
Difficult life experiences can translate to an increase in the stress hormones in our bodies. And that can make the asthma symptoms more severe or more frequent.”
What can I do to protect my child from the effects of traumatic experiences?
We can teach kids to find their words and talk through their emotions, which can help them calm down and regulate. This can sometimes help their asthma get better. It might sound a little strange, but there’s science behind it.”
What are some resources that I can use to talk to my child?
First of all, you are the biggest resource. You, yourself and that strong bond that you have with your kids is the strongest foundation and the best thing. You already have that trust and that bond.
Sometimes it can be helpful to have an activity to do together where we’re able to talk about these difficult experiences. One activity that I like to use for kids this age are books. There’s a wonderful book, called Once I Was Very, Very Scared. It’s a beautifully illustrated book that’s available for free online. You can incorporate it into your bedtime routine. It’s a story about how different animals living in a forest together react when they’re scared or angry.
I really like using this as a way to talk about emotions. Then you can point at the book and say, “Have you ever felt like that? Do you ever feel like the skunk, and you just want to spray things away?
Lastly, I have a magic wand, and it’s got little glitter stars and hearts in here. This can be a good way to teach kids about a lot of different things. My favorite way to use it is for deep breathing. If you have one like this at home, or anything that’s really just kind of mesmerizing to look at, you can practice saying, “Okay, when I’m feeling a little overwhelmed and I don’t know what to do, you can pull out your object, and then you take a big deep breath and try to follow one single piece of glitter.” We call it a grounding exercise, and it’s a great way to help a child temper down and take a big, deep breath as they’re trying to re-regulate their emotions.”
Reflective Practices
Self Reflection
Now that you’ve reviewed the scenario above, reflect on the questions here, either on your own or in a group setting:
- How do you think that went?
- What do you think went well and what could have been improved?
- What language could you see yourself using when conducting an ACEs screening?
- How might this scenario be different if it were in person rather than telehealth?
Mentoring Moments
After you’ve had a chance to reflect on your own, view a conversation between the health care team and Dr. Alicia Lieberman, Professor of Psychiatry at UCSF and Director of the Child Trauma Research Program.
Now You Try It
Note: This is intended for all members of the health care team. Remember that we’re all learning and that there are no mistakes.
Review
- Find the words and the body language from the Watch and Learn section that feel comfortable for you and that you can envision using in your conversations with patients.
- Jot down some of the suggestions from the Reflective Practice section that were most helpful to you.
- Now take a moment and visualize yourself running through this scenario with a patient.
Practice
Remember that we’re all learning and that there are no mistakes.
- On your own or with another person, practice using the words and the body language that convey the message that you want. Alternatively, you can record a voice memo or video on your phone so that you can play it back to review. You may also get feedback from a trusted colleague or friend.
- In a group setting, pair-share or self-reflection, consider these questions:
- What came easy to you? What would take some work?
- What do you think you are doing well?
- What do you need some practice with?